- Over 80 percent of non-small cell lung cancer detected at Stage 4
- Fewer than 50 percent of patients had five or more biomarker tests
- Median time from diagnosis to first-line therapy is about five weeks
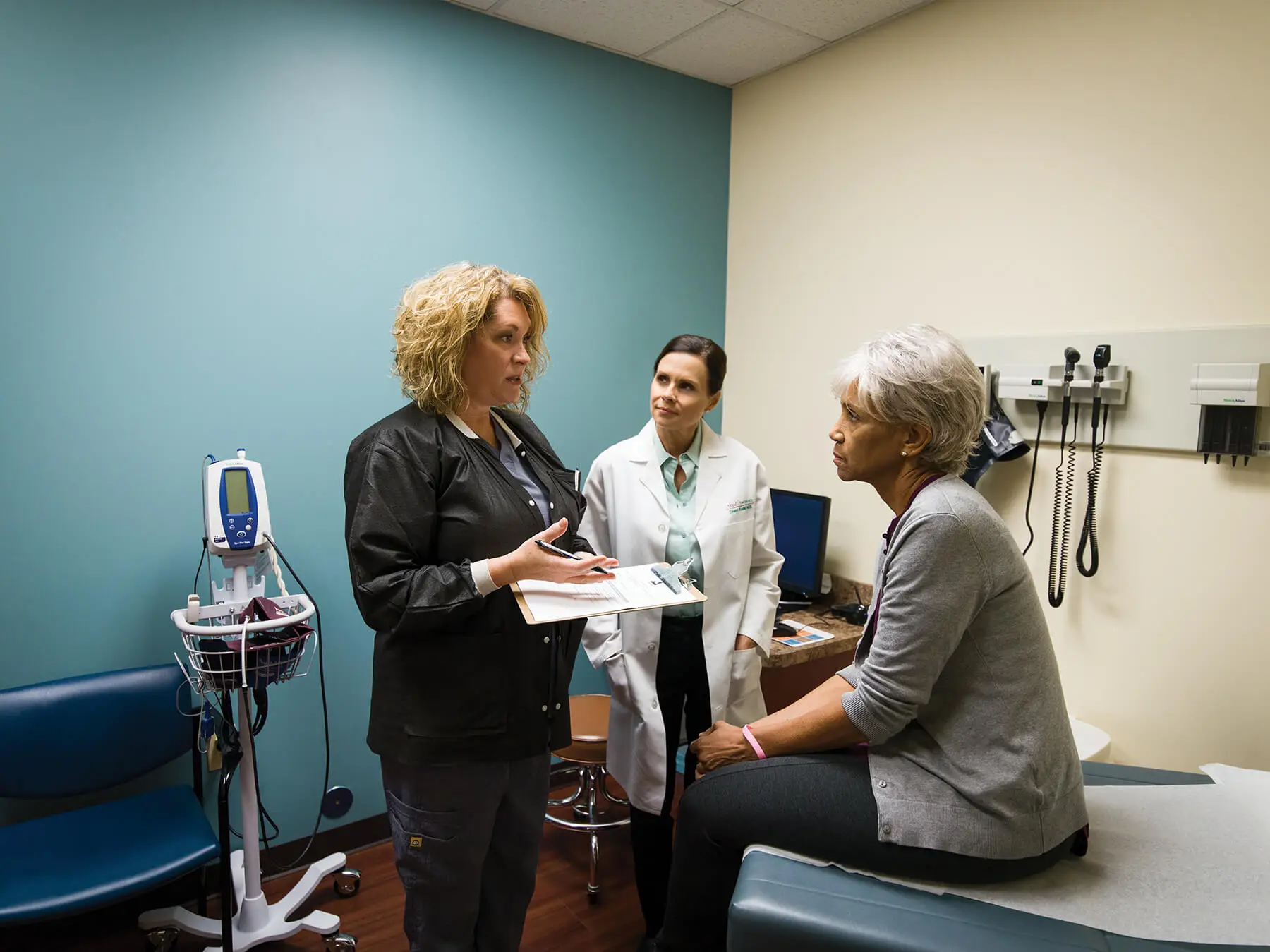
THE WOODLANDS, TEXAS, June 4, 2021 — Results from the first phase of the broad, collaborative MYLUNG ConsortiumTM research study in metastatic non-small cell lung cancer (mNSCLC) were released by The US Oncology Network (The Network), US Oncology Research and OntadaTM at the 2021 American Society of Clinical Oncology (ASCO) Annual Meeting. The findings provide a close-up look at current biomarker testing rates and turnaround times for patients with mNSCLC treated in community practices within The Network. Most notably, Protocol 1 findings show that there are barriers that must be addressed as more than 80 percent of NSCLC is detected at Stage 4 and median time from diagnosis to first-line therapy is about five weeks.
“The pace and development of treatments in non-small cell lung cancer is dramatic,” said Makenzi Evangelist, MD, principal investigator for the MYLUNG Consortium’s Protocol 2 and oncologist with New York Oncology Hematology (NYOH), a practice in The Network. “There are already several targeted therapies to treat subsets of populations, and many more are in the pipeline that hold incredible potential. Unfortunately, barriers exist that prevent the necessary comprehensive biomarker testing that enables the use of these treatments. The MYLUNG Consortium study will be invaluable in identifying these obstacles and developing practical interventions that will allow us to fulfill the promise of precision medicine for patients with this difficult cancer.”
Dr. Evangelist presented the findings during an oral presentation at ASCO titled, “Biomarker tissue journey among patients with untreated metastatic non-small cell lung cancer (mNSCLC) in The US Oncology Network community practices.” (ASCO Abstract 9004).
The MYLUNG Consortium is a collaborative and innovative research study comprised of three protocols over a five-year period. Protocol 1, which was just completed, is a retrospective study of more than 3,500 patients with mNSCLC that investigated the following areas: testing rates for ALK, BRAF, EGFR, ROS1, and PD-L1 mutations; use of the full next-generation sequencing panel (NGS); time from NSCLC diagnosis to first-line therapy; turnaround times from biomarker orders to results; and time from NSCLC diagnosis to test results.
“We have derived significant insights from the study data so far,” noted Sarah Alwardt, PhD, vice president of Operations for Ontada. “We are now able to see where there are gaps regarding targeted therapy. This real-world study showed that while most patients had at least one biomarker test result available prior to first-line therapy, less than 50 percent had five or more biomarkers tested. Consequently, a large percentage of patients were not given the opportunity for a targeted therapy.”
Additionally, the median time from diagnosis to first-line therapy was about five weeks, a concern for patients anxiously waiting for treatment. Turnaround time from testing orders to results was about two weeks, indicating the need to get test results to physicians sooner so they have all critical information in front of them during development of the treatment plan. Next Generation Sequencing testing improved over time, suggesting comprehensive testing is increasing. Most of the population was diagnosed at advanced disease, with roughly over 80 percent detected at stage 4.
“Protocol 1 provides a look at what was happening retrospectively based on clinical data abstraction, allowing us to draw some early conclusions about historical baseline trends for testing patterns,” noted Robert L. Coleman, MD, FACOG, FACS, chief scientific officer of US Oncology Research and the MYLUNG Consortium program principal investigator. “Retrospective studies like this help us understand where we are as far as testing behaviors, while also identifying gaps in the data that need to be filled with the prospective research the MYLUNG Consortium will address in the next protocols.”
Data from Protocol 1 will be compared to the next phase of the MYLUNG Consortium study, Protocol 2, which will evaluate contemporary ordering practices and turnaround times prospectively. It will enroll about 1,000 patients from approximately 11 sites and will monitor the real-world patient journey from presentation through their first line of cancer therapy, focusing on how diagnostic biomarker information is obtained, utilized and operationalized in decision-making. Patients are currently being enrolled in this stage of the study.
The final phase of the study, Protocol 3, will serve as a platform upon which prospectively assessed interventional strategies in patient-engagement algorithms will be conducted. Up to 7,500 patients from approximately 20 participating sites will be recruited over a five-year period. Individual clinical trials will integrate findings from the previous protocols and explore new processes and associated outcomes. The goal is to help providers make the best treatment recommendations based on the data available while improving access to testing and appropriate therapies for patients with mNSCLC.
The MYLUNG Consortium study is enabled through a unique collaboration of various organizations and stakeholders working together across the spectrum of NSCLC drug development, therapy and care. The number of consortium participants continues to grow, all bringing unique perspectives to this innovative study. It brings together providers and researchers in The Network, US Oncology Research and Ontada with life sciences companies Amgen, AstraZeneca, Eli Lilly and Company, Genentech (a member of the Roche Group), and Mirati Therapeutics, Inc. Patient advocacy groups LUNGevity and GO2 Foundation for Lung Cancer are also participating, playing a key role in the study by keeping the focus on patients. Healthcare provider members include Illinois Cancer Specialists, Maryland Oncology Hematology, Minnesota Oncology, New York Oncology Hematology, Oncology Hematology Care, Rocky Mountain Cancer Centers, Southern Cancer Center, Virginia Cancer Specialists, Virginia Oncology Associates, Willamette Valley Cancer Institute and Research Center and Woodlands Medical Specialists.
Read more about the MYLUNG Consortium here. To schedule a media interview with one of the study investigators, contact Claire Crye at Claire.Crye@usoncology.com.
###
About The US Oncology Network
Every day, The US Oncology Network (The Network) helps approximately 1,400 independent physicians deliver value-based, integrated care to patients — close to home. Through The Network, these independent doctors come together to form a community of shared expertise and resources dedicated to advancing local cancer care and to delivering better patient outcomes. The Network provides practices with access to coordinated resources, best business practices, and the experience, infrastructure and support of McKesson Corporation. This collaboration allows the providers in The Network to focus on the health of their patients, while McKesson focuses on the health of their practices. The Network is committed to the success of independent practices, everywhere.
About US Oncology Research
US Oncology Research draws from a network of experienced investigators and dedicated clinical staff who specialize in oncology clinical trials. US Oncology Research serves approximately 60 research sites and more than 165 locations, managing about 400 active trials at any given time. For the past 20 years, physicians in the research network have enrolled more than 85,000 patients in over 1,600 trials and have played a role in more than 100 FDA-approved cancer therapies. US Oncology Research is supported by McKesson Corporation.
About Ontada
OntadaTM is an oncology data, research and technology business dedicated to improving the lives of cancer patients. Part of McKesson Corporation, we partner with life science companies to support science through real-world data and evidence, helping to accelerate drug development and commercialization, connect community oncology providers to educational programs that enable them to practice at the forefront of therapies, and advance precise, evidence-driven patient care through practice technologies in the community setting. For more information, visit ontada.com or follow @OntadaOncology.
Key highlights include a plenary session on cervical cancer among women in developing nations and an oral abstract exploring molecular testing and targeted therapy for metastatic non-small cell lung cancer, among other topics
THE WOODLANDS, Texas, June 3, 2021 — US Oncology Research, The US Oncology Network (The Network), and OntadaTM announce they contributed to more than 75 studies covering topics including gynecologic cancer, lung cancer and immunotherapy which will be presented at the upcoming 2021 American Society of Clinical Oncology (ASCO) Annual Meeting, to be held virtually from June 4 – 8.
“At this year’s ASCO Annual Meeting, we are looking forward to sharing our latest insights and knowledge across the global oncology community,” said Robert L. Coleman, MD, chief scientific officer, US Oncology Research. “As we emerge from a year that challenged how we approach the fight against cancer, it is more important than ever to discuss how we can work together to ensure this next chapter of commitment to equitable care and innovation.”
Key highlights include a plenary session exploring the role of adjuvant chemotherapy following chemoradiation in women with cervical cancer, featuring results from OUTBACK, a randomized Phase III trial to determine if the addition of adjuvant chemotherapy to standard cisplatin-based chemoradiation improves rates of overall survival. The plenary session, which will be held Sunday, June 6 from 1 -4 p.m. ET, will feature abstract LBA3, “Adjuvant chemotherapy following chemoradiation as primary treatment for locally advanced cervical cancer compared to chemoradiation alone: The randomized phase III OUTBACK Trial.”
“Despite the recently developed cervical cancer vaccine, many women will continue to die from this disease if existing treatments are not improved,” said Bradley Monk, MD, FACOG, FACS, co-author of the study and oncologist with Arizona Oncology, a practice in The Network. “We are eager to present the results from this featured late-breaking plenary and to draw attention to the problem of cervical cancer among women in developing nations.”
Also of note this year are findings from the MYLUNG ConsortiumTM study, which will be featured in an oral abstract session. Given the importance of molecular testing and targeted therapy for metastatic non-small cell lung cancer, the findings provide an assessment of real-world biomarker testing rates and turnaround times of more than 1,000 providers across the U.S. The session titled, “Lung Cancer—Non-Small Cell Metastatic,” will be held Friday, June 4 from 1 – 4 p.m. ET and will feature abstract 9004, “Biomarker tissue journey among patients (pts) with untreated metastatic non-small cell lung cancer (mNSCLC) in The US Oncology Network community practices.”
“While treatment decisions based on molecular analyses can improve outcomes, many patients do not undergo timely comprehensive testing,” said Makenzi Evangelist, MD, study co-author, principal investigator for Protocol 2 of the MYLUNG Consortium and oncologist with New York Oncology Hematology (NYOH), a practice in The Network. “Through this real-world analysis, we observed that less than half of patients with mNSCLC had five or more biomarkers tested before initiating first-line systemic therapy. These findings deepen our understanding of the barriers patients face and help us target new approaches for improving their care.”
“Through the MYLUNG Consortium, we are able to bring together providers, life sciences companies and patient advocacy groups with a common goal of improving patient outcomes,” added Dr. Coleman, who is the MYLUNG Consortium program principal investigator. “What we are presenting at this year’s ASCO Annual Meeting are findings from Protocol 1. This innovative study will last five years with about 20 participating sites recruiting up to 12,000 patients.”
“This study was the first real-world study that analyzed the incorporation of immunotherapy in the treatment of small cell lung cancer,” said Eric Nadler, MD, MPP, study co-author and oncologist with Texas Oncology, a practice in The Network. “Being able to leverage real-world data into today’s clinical research is a huge step forward. We now have the ability to take a plethora of already available and extremely valuable data and study thousands of patient journeys for numerous indications.”
Ontada President Susan Shiff, PhD, MBA, concludes, “We are excited to present the results of studies that have used a variety of retrospective and prospective methodologies whose findings can help to improve the lives of cancer patients, which of course is our ultimate goal.”
You can find the full schedule of affiliated data presentations from US Oncology Research, The US Oncology Network and Ontada at ASCO this year, including author details, here. For more information or to interview a trial investigator, contact Claire Crye at 281.825.9927 or Claire.Crye@usoncology.com, or Edie DeVine at 209.814.9564 or Edie.DeVine@gcihealth.com.
###
About US Oncology Research
US Oncology Research draws from a network of experienced investigators and dedicated clinical staff who specialize in oncology clinical trials. US Oncology Research serves approximately 60 research sites and more than 165 locations, managing about 400 active trials at any given time. For the past 20 years, physicians in the research network have enrolled more than 85,000 patients in over 1,600 trials and have played a role in more than 100 FDA-approved cancer therapies. US Oncology Research is supported by McKesson Corporation.
About The US Oncology Network
Every day, The US Oncology Network (The Network) helps approximately 1,400 independent physicians deliver value-based, integrated care to patients — close to home. Through The Network, these independent doctors come together to form a community of shared expertise and resources dedicated to advancing local cancer care and to delivering better patient outcomes. The Network provides practices with access to coordinated resources, best business practices, and the experience, infrastructure and support of McKesson Corporation. This collaboration allows the providers in The Network to focus on the health of their patients, while McKesson focuses on the health of their practices. The Network is committed to the success of independent practices, everywhere.
About Ontada
OntadaTM is an oncology data, research and technology business dedicated to improving the lives of cancer patients. Part of McKesson Corporation, we partner with life sciences companies to support science through real-world data and evidence, helping to accelerate drug development and commercialization, connect community oncology providers to educational programs that enable them to practice at the forefront of therapies, and advance precise, evidence-driven patient care through practice technologies in the community setting. For more information, visit ontada.com or follow @OntadaOncology.
By joining The Network, these physicians contribute to the expansion of colorectal services in Texas
THE WOODLANDS, Texas, April 1, 2021—The US Oncology Network (The Network), the largest organization of its kind dedicated to advancing local cancer care and better patient outcomes, continues to expand its reach into local communities while broadening its surgical expertise with the addition of physicians from Texas Colon & Rectal Specialists (TCRS), a large colorectal practice in North Texas, as a part of Texas Oncology, a practice in The Network. The addition brings 17 new surgical specialists into The Network, greatly strengthening the organization’s expertise and knowledgebase in surgical specialties. The Network now has more than 200 surgical specialists, covering a wide range of specialties including: Gynecologic Oncology, Breast Surgery, Urology, Surgical Oncology, Colorectal Surgery, Thoracic Surgery, Orthopedic Oncology Surgery, Plastic Surgery and Head and Neck Surgery.
“With the addition of the physicians from TCRS, we have more than doubled the number of surgical specialists focused on colorectal surgery in The Network,” said Michael V. Seiden, MD, PhD, president, The US Oncology Network. “These physicians are meeting a critical need in cancer care, as colon cancer is the second leading cause of cancer deaths in the United States for men and women combined. While the increase in this specialty is dramatic, we are continuing to see accelerated growth in all disciplines as physicians look to The Network to help them cope with the increasingly challenging healthcare environment.”
The TCRS physicians typify physicians who have recently joined The Network, driven by the increasing complexity of the healthcare landscape and the impact of COVID-19. Within the past year, The Network welcomed 131 new physicians and 22 advanced practice providers into the organization, significantly increasing the availability of advanced cancer care in local communities while strengthening these providers’ ability to remain independent and viable.
More and more physicians are turning to The Network to leverage the many benefits that empower practices to succeed during uncertain times. Access to experts in community care, clinical and business consulting services, and innovative technologies that support high-quality care, efficient drug management, and revenue cycle optimization enable practices to successfully meet constantly changing challenges. Practices can also access Value Pathways powered by NCCN™—evidence-based treatment guidelines developed by physicians and clinicians in The Network along with the National Comprehensive Cancer Network®. As part of The Network, providers can also collaborate with more than 1,900 physicians and clinicians, sharing expertise and best practices. Additionally, The Network advocates for and negotiates with payers, legislators and manufacturers, leveraging its substantial resources on behalf of member practices.
“Joining Texas Oncology and uniting with The US Oncology Network provides us tremendous value, giving us access to vast resources and expertise,” said Dale Burleson, M.D., medical director of Texas Oncology’s new colorectal surgery division. “We are excited to benefit from the many services and technologies The Network offers that will allow us to continue to focus on providing our patients with high-quality care and optimal outcomes.”
The 17 board-certified single-specialty colorectal physicians are experts in the surgical and non-surgical treatment of colon and rectal problems. They have exceptional credentials, proven experience and prominent reputations in the medical community. As innovators in advanced colorectal care, the physicians performed more robotic, laparoscopic and minimally invasive colorectal procedures than any other practice in North Texas. They are also intimately involved in training and equipping the next generation of colorectal physicians. With 19 convenient locations that span several counties, most patients will not have far to travel for care.
“The addition of TCRS physicians provides benefits to Texas Oncology, most notably our ability to provide patients accessibility to high-quality, colorectal care right in their own communities and more opportunities to participate in value-based care opportunities, outcomes benchmarking and development of best practices, as well as groundbreaking clinical trials and research,” said R. Steven Paulson, MD, practice president, Texas Oncology. “Their expertise will be invaluable as we collaborate across our practice and The Network to advance care for colorectal diseases and disorders.”
###
About The US Oncology Network
Every day, The US Oncology Network (The Network) helps more than 1,380 independent physicians deliver value-based, integrated care to patients — close to home. Through The Network, these independent doctors come together to form a community of shared expertise and resources dedicated to advancing local cancer care and to delivering better patient outcomes. The Network provides practices with access to coordinated resources, best business practices, and the experience, infrastructure and support of McKesson Corporation. This collaboration allows the providers in The Network to focus on the health of their patients, while McKesson focuses on the health of their practices. The Network is committed to the success of independent practices, everywhere.
Contact
The US Oncology Network
Claire Crye, Public Relations
281.825.9927 claire.crye@usoncology.com
Eight custom measures receive approval, raising the bar on oncology patient care
IRVING, Texas, March 25, 2021 — For the fifth consecutive year, McKesson has received approval from The Centers for Medicare & Medicaid Services (CMS) to participate in the Merit-based Incentive Payment System (MIPS) as a Qualified Clinical Data Registry (QCDR). As a CMS-approved QCDR, Practice Insights, a practice performance analytics tool powered by McKesson’s new oncology technology and insights business Ontada, can collect and report clinical data on behalf of clinicians for both MIPS and custom QCDR quality measures to drive improvements in quality and cost of care. The designation enables iKnowMed℠ electronic health record (EHR) users to efficiently submit data directly to CMS without engaging a separate registry vendor, streamlining data submission and minimizing the need for additional administrative resources.
In addition, CMS approved all eight of the custom QCDR measures developed by The US Oncology Network and submitted as part of McKesson’s 2021 application, confirming the importance of these measures to the quality and integrity of oncology care.
“As a QCDR, we are pleased to be recognized as a CMS-approved organization that collects, reports and analyzes medical data with the ultimate aim to improve the quality of patient care,” said Marcus Neubauer, MD, chief medical officer of The US Oncology Network, a network supported by McKesson of more than 1,380 independent, community-based physicians. “The approval of eight quality measures that we submitted is a success as much for our organization as for the entire field of oncology and for value-based care, as these measures help raise the bar on patient care while also addressing cost.”
The eight oncology-specific custom QCDR measures submitted by McKesson and approved by CMS include:
- Advance care planning in patients with metastatic cancer
- Patient-reported pain improvement
- Mutation testing for lung cancer completed prior to start of targeted therapy
- Supportive care drug utilization in last 14 days of life
- Hepatitis B serology testing and prophylactic treatment prior to receiving anti-CD20 targeting drugs
- Utilization of PET, PET/CT or CT scans for breast cancer stage 0, I or II at any time during the course of evaluation and treatment
- Utilization of GCSF in metastatic colorectal cancer
- Combination chemotherapy recommended or received within 4 months of diagnosis by women under 70 with AJCC stage T1cN0M0 to Stage 1B-III ER/PR negative breast cancer
“CMS continues to raise the standard for QCDR measure approval, with the goal of encouraging the measures that matter most to improving quality patient care,” said Lalan Wilfong, MD, vice president of Value-Based Care and Quality Programs for Texas Oncology, a practice in The US Oncology Network. “Our ultimate goal is to utilize quality measures to improve the care we provide. It’s also important to limit the number of measures in the MIPS program to ease the reporting burden on clinicians and reduce the overall cost of care. For these reasons, we took great care in developing the custom measures, submitting a wealth of supporting data and research to support our case. The approval of each measure from CMS is a validation of the hard work, clinical acumen and patient-first mindset of our team, and we are honored to be part of this important work moving cancer care forward.”
Along with The US Oncology Network, McKesson also supports oncology practices through its Onmark group purchasing organization (GPO), and the QCDR measure approvals reflect the organization’s insight into the entire landscape of oncology care.
“I am extremely proud of the work we do to shepherd both The Network and Onmark practices along the value-based care continuum,” said Erin Crum, director, Quality Measurement Strategy, McKesson. “Thanks to the collaborative efforts of diverse teams across McKesson, we are able to deliver reporting that is critical to oncology practices’ value-based care success.”
###
About McKesson Corporation
McKesson Corporation is a global leader in healthcare supply chain management solutions, retail pharmacy, community oncology and specialty care, and healthcare information solutions. McKesson partners with pharmaceutical manufacturers, providers, pharmacies, governments and other organizations in healthcare to help provide the right medicines, medical products and healthcare services to the right patients at the right time, safely and cost-effectively. United by our ICARE shared principles, our employees work every day to innovate and deliver opportunities that make our customers and partners more successful – all for the better health of patients. McKesson has been named the “Most Admired Company” in the healthcare wholesaler category by FORTUNE, a “Best Place to Work” by the Human Rights Campaign Foundation, and a top military-friendly company by Military Friendly. For more information, visit www.mckesson.com.
About The US Oncology Network
Every day, The US Oncology Network (The Network) helps more than 1,380 independent physicians deliver value-based, integrated care to patients — close to home. Through The Network, these independent doctors come together to form a community of shared expertise and resources dedicated to advancing local cancer care and to delivering better patient outcomes. The Network provides practices with access to coordinated resources, best business practices, and the experience, infrastructure and support of McKesson Corporation. This collaboration allows the providers in The Network to focus on the health of their patients, while McKesson focuses on the health of their practices. The Network is committed to the success of independent practices, everywhere.
About Ontada
Ontada is an oncology technology and insights business dedicated to transforming the fight against cancer. Part of McKesson Corporation, Ontada was founded on the core belief that precise insights – delivered exactly at the point of need – can save more patients’ lives. We connect the full patient journey by combining technologies used by The US Oncology Network and other community oncology providers with real-world data and research relied on by all top 15 global life sciences companies. Our work helps accelerate innovation and power the future of cancer care. For more information, visit ontada.com or follow @OntadaOncology.
Media Contact
McKesson
Claire Crye, Public Relations
281.825.9927 claire.crye@mckesson.com
Unique, collaborative real-world research consortium will study up to 12,000 NSCLC patients in the community setting over five years
MYLUNG to deepen understanding of barriers and address challenges to improve care for lung cancer patients, including those with targetable mutations
The MYLUNG consortium – or “Molecularly Informed Lung Cancer Treatment in a Community Cancer Network: A Pragmatic Consortium” – will observe up to 12,000 community-based, metastatic NSCLC patients over a five-year period in one of the first broad, collaborative, research endeavors in lung cancer. In particular, MYLUNG aims to deepen understanding of molecular testing barriers to improve care for lung cancer patients, including those with mutations who may benefit from receiving precision medicine, the practice of leveraging targeted therapies across the continuum of care, as well as expand the opportunity for patients to participate in clinical trials.
“Many patients are not receiving the molecular testing they need to initiate targeted therapy early in their cancer care journey due to long timeframes, lack of coverage or another factor. This testing is critical to determine the patient’s cancer at a molecular level, so oncologists can create a more targeted and precise treatment plan,” said Robert L. Coleman, MD, FACOG, FACS, chief scientific officer, US Oncology Research. “In order to fulfill the promise of precision medicine for NSCLC patients, we need a fuller understanding of the barriers, challenges, risks and opportunities around molecularly guided therapies. MYLUNG will draw insights from these datasets that can lead to better therapy for patients in a timelier manner.”
Lung cancer treatment is becoming increasingly personalized to include targeted therapies into earlier stages of disease. To support this, MYLUNG provides the framework to conduct research studies that will help define best practices for providers, as well as provide insights for life sciences companies seeking to quickly deliver potentially life-saving treatments to the patients who need them.
The MYLUNG consortium brings together several McKesson-supported organizations focused on transforming and enhancing the cancer care experience including The US Oncology Network, US Oncology Research, and OntadaTM – McKesson’s new oncology technology and insights business – along with life sciences companies and patient advocacy groups. MYLUNG life sciences members currently include Amgen, Eli Lilly and Company and Mirati Therapeutics. Healthcare provider members include Illinois Cancer Specialists, Maryland Oncology Hematology, Minnesota Oncology, New York Oncology Hematology, Oncology Hematology Care, Rocky Mountain Cancer Centers, Southern Cancer Center, Virginia Cancer Specialists, Virginia Oncology Associates and Willamette Valley Cancer Institute and Research Center. Additional collaborators are expected to join throughout the next few months.
“McKesson has always served at the center of care delivery, which has provided a unique perspective on the complexities of cancer care and the growing needs among providers and life sciences companies,” said Kirk Kaminsky, president, McKesson U.S. Pharmaceutical. “MYLUNG highlights our ability to integrate a continuous virtual cycle with feedback loops between the US Oncology Research and Ontada research teams and The US Oncology Network sites of care to quickly integrate best practices across The Network, while adaptively responding to the constantly changing landscape of oncology discovery for both diagnostics and treatment.”
MYLUNG will consist of three protocols over a five-year period:
- Protocol 1 retrospectively reviews real-world data from Ontada’s iKnowMedSM electronic health records (EHRs) of about 3,500 patients treated by providers in The US Oncology Network to understand baseline data on molecular testing across practices and identify historical barriers to testing and precision medicine in community practice.
- Protocol 2, enrolling about 1,000 patients from approximately 10 practices, will monitor the real-world patient journey from presentation through their first line of cancer therapy, focusing on how diagnostic biomarker information is obtained, utilized and operationalized in decision-making. Patients are currently being enrolled into Protocol 2.
The real-world research model is uniquely suited to take lung cancer care to the next level by providing a window into the actual provider and patient experience. “We created Ontada to help providers, patients and life sciences companies navigate a cancer care world that is growing more complex every day as new precision medicines come to market,” said Derek Rago, interim president, Ontada. “MYLUNG will gather real-world data with Ontada’s technology solutions and develop novel insights through its real-world analytics capabilities so that all stakeholders can make informed decisions that are actionable at the point-of-need.”
MYLUNG is poised to support meaningful progress and innovation in care delivery and potentially touch and improve thousands of lives. Makenzi Evangelist, MD, physician lead for the pragmatic study and oncologist with New York Oncology Hematology (NYOH), a practice in The Network, said, “During the study and after, we hope that the interventions and our understanding of NSCLC improve, and we see increased testing and appropriate use of targeted therapies – all of which we hope will improve cancer care and patient outcomes.”
###
About McKesson Corporation
McKesson Corporation is a global leader in healthcare supply chain management solutions, retail pharmacy, community oncology and specialty care, and healthcare information solutions. McKesson partners with pharmaceutical manufacturers, providers, pharmacies, governments and other organizations in healthcare to help provide the right medicines, medical products and healthcare services to the right patients at the right time, safely and cost-effectively. United by our ICARE shared principles, our employees work every day to innovate and deliver opportunities that make our customers and partners more successful – all for the better health of patients. McKesson has been named the “Most Admired Company” in the healthcare wholesaler category by FORTUNE, a “Best Place to Work” by the Human Rights Campaign Foundation, and a top military-friendly company by Military Friendly. For more information, visit www.mckesson.com.
About Ontada
Ontada is an oncology technology and insights business dedicated to transforming the fight against cancer. Part of McKesson Corporation, Ontada was founded on the core belief that precise insights – delivered exactly at the point of need – can save more patients’ lives. We connect the full patient journey by combining technologies used by The US Oncology Network and other community oncology providers with real-world data and research relied on by all top 15 global life sciences companies. Our work helps accelerate innovation and power the future of cancer care. For more information, visit ontada.com or follow @OntadaOncology.
About US Oncology Research
US Oncology Research draws from a network of experienced investigators and dedicated clinical staff who specialize in oncology clinical trials. US Oncology Research serves approximately 60 research sites and more than 165 locations, managing about 400 active trials at any given time. For the past 20 years, physicians in the research network have enrolled more than 82,000 patients in over 1,600 trials and have played a role in more than 100 FDA-approved cancer therapies. US Oncology Research is supported by McKesson Corporation.
About The US Oncology Network
Every day, The US Oncology Network (The Network) helps more than 1,380 independent physicians deliver value-based, integrated care to patients — close to home. Through The Network, these independent doctors come together to form a community of shared expertise and resources dedicated to advancing local cancer care and to delivering better patient outcomes. The Network provides practices with access to coordinated resources, best business practices, and the experience, infrastructure and support of McKesson Corporation. This collaboration allows the providers in The Network to focus on the health of their patients, while McKesson focuses on the health of their practices. The Network is committed to the success of independent practices, everywhere.
Media Contacts
The US Oncology Network, US Oncology Research
Claire Crye, Public Relations
281.825.9927 claire.crye@mckesson.com
Ontada
Annabelle Baxter, External Communications
469.233.3400 annabelle.baxter@mckesson.com
Top researchers to present the latest clinical findings advancing treatment options for blood cancers and other hematologic diseases
THE WOODLANDS, Texas, Dec. 2, 2020 — During the 62nd American Society of Hematology (ASH) Annual Meeting and Exposition, principal investigators from The US Oncology Network (The Network) and US Oncology Research will share detailed results from 30 studies covering topics that include Hodgkin lymphoma, multiple myeloma and the effects of cancers on older patient populations. The ASH Annual Meeting, a leading scientific event in malignant and non-malignant hematology, will be taking place virtually from Dec. 5-8, 2020.
“In this landscape impacted by COVID-19, real-world evidence shows that our collective fight against cancer must include advancing clinical research and empowering patients through timely health screenings,” said Robert L. Coleman, MD, chief scientific officer, US Oncology Research. “At this year’s ASH virtual meeting, we are looking forward to sharing the latest advances from investigators in The Network and to exploring ways we can continue working together to navigate the unprecedented challenges and risks that patients with cancer are facing today.”
Christopher A. Yasenchak, MD, associate chair of hematology research for US Oncology Research and a hematologist with Willamette Valley Cancer Institute and Research Center, will present an oral abstract titled, “Frontline Brentuximab Vedotin as Monotherapy or in Combination for Older Hodgkin Lymphoma Patients,” on Sunday, Dec. 6, at 2:15 p.m. ET.
“Older patients with Hodgkin lymphoma often have poorer outcomes than younger patients due to comorbidities and the toxicity of conventional first-line chemotherapy,” said Dr. Yasenchak. “Brentuximab vedotin, as monotherapy and in combination with other agents, shows high response rates and clinically meaningful improvements in progression-free survival and tolerability compared to conventional combination chemotherapy. The study, SGN35-015, presents compelling evidence underscoring the growing interest and urgency in research to advance cancer treatment and care for older populations.”
In addition, Robert Rifkin, MD, FACP, medical director of biosimilars for McKesson, associate chair of hematology research and myeloma disease lead for US Oncology Research and a hematologist with Rocky Mountain Cancer Centers, a practice in The Network, co-authored “The Phase 3 TOURMALINE-MM2 Trial: Oral Ixazomib, Lenalidomide, and Dexamethasone (IRd) Vs Placebo-Rd for Transplant-Ineligible Patients With Newly Diagnosed Multiple Myeloma (NDMM).” The oral presentation will take place on Monday, Dec. 7, at 7:45 a.m. ET.
“Patients who are newly diagnosed with multiple myeloma and not eligible for autologous stem cell transplants need additional treatment options,” said Dr. Rifkin. “We believe the findings from TOURMALINE-MM2 emphasize the need for all-oral, proteasome inhibitor-based treatment options and will help pave the way for future innovation on behalf of the multiple myeloma community.”
Dr. Rifkin will also present a trial-in-progress poster, “DREAMM-7: A Phase III Study of the Efficacy and Safety of Belantamab Mafodotin (Belamaf) With Bortezomib, and Dexamethasone (B-Vd) in Patients with Relapsed/Refractory Multiple Myeloma (RRMM),” on Monday, Dec. 7, from 7:00 a.m.–3:30 p.m. ET.
Another oral abstract, “Subgroup Analyses of Elderly Patients Aged ≥ 70 Years in MAGNIFY: A Phase IIIb Interim Analysis of Induction R2 Followed By Maintenance in Relapsed/Refractory Indolent Non-Hodgkin Lymphoma,” was co-authored by David Andorsky, MD, a hematologist with Rocky Mountain Cancer Centers. The presentation will take place on Sunday, Dec. 6, at 10:30 a.m. ET.
“Results from MAGNIFY indicate an important option for older, high-risk patients with non-Hodgkin lymphoma who have relapsed or did not respond to previous treatment with chemotherapy,” said Dr. Andorsky. “In this patient population, lenalidomide combined with rituximab—with close attention to dose reduction—demonstrated encouraging efficacy and a tolerable safety profile.”
Mitul Gandhi, MD, a medical oncologist with Virginia Cancer Specialists, a practice in The Network, co-authored the poster, “Safety and Antitumor Activity Study Evaluating Loncastuximab Tesirine and Rituximab Versus Immunochemotherapy in Diffuse Large B-Cell Lymphoma.” The presentation will take place on Sunday, Dec. 6, from 7:00 a.m.–3:30 p.m. ET.
“Options are critically needed to improve outcomes for patients with diffuse large B-cell lymphoma who did not respond to previous therapy, are unsuitable for autologous stem cell transplantation or relapsed shortly after a transplantation,” said Dr. Gandhi. “I am looking forward to presenting findings that indicate the potential to meet the needs of more patients with this aggressive form of lymphoma.”
Furthermore, Houston Holmes, MD, a medical oncologist and hematologist at Texas Oncology, a practice in The Network, co-authored the oral abstract “Single-Agent Mosunetuzumab Is a Promising Safe and Efficacious Chemotherapy-Free Regimen for Elderly/Unfit Patients With Previously Untreated Diffuse Large B‑Cell Lymphoma.” The presentation will take place on Sunday, Dec. 6, at 12:15 p.m. ET.
“Among patients with diffuse large B-cell lymphoma, approximately 30% over age 75 do not receive standard chemotherapy as a first-line treatment due to concerns about frailty and comorbidities,” said Dr. Holmes. “Based on early clinical data, single-agent mosunetuzumab could offer a promising chemotherapy-free regimen for these patients who otherwise have limited options.”
Researchers with McKesson Data, Evidence and Insights also worked with US Oncology Research and The US Oncology Network physicians on studies advancing the applications of real-world evidence, which will be presented this year.
Dr. Yasenchak will present a real-world evidence study titled, “Real-World Adherence to National Comprehensive Cancer Network (NCCN) Guidelines Regarding the Usage of PET/CT and Reported Deauville Scores in Advanced Stage Classical Hodgkin Lymphoma: A Community Oncology Practice Perspective.” The poster presentation will take place on Sunday, Dec. 6, from 7:00 a.m.–3:30 p.m. ET.
“Providers may not always have the comprehensive information needed to optimize treatment modifications for patients with Hodgkin lymphoma,” added Dr. Yasenchak. “Based on our findings, there is an opportunity to educate oncologists and radiologists about the importance of consistently reporting PET/CT Deauville scores in the initial staging and assessment of treatment response for these patients.”
An additional real-world evidence poster, “NHL Patients and Nurses in the US Prefer Subcutaneous Rituximab Injection Versus Intravenous Rituximab Infusion: A Real-World Study,” will be presented by Dr. Gandhi on Saturday, Dec. 5 from 7:00 a.m.–3:30 p.m. ET.
“As the COVID-19 pandemic adds new barriers to our health systems and the completion of clinical trials, real-world evidence is pivotal in providing insights into how we can improve outcomes,” said Nicholas J. Robert, MD, medical director, McKesson Data, Evidence and Insights. “By leveraging data from our electronic medical records, healthcare providers and researchers are making an impact and optimizing care for patients managing cancer.”
The full schedule of affiliated data presentations, including timing and author information, can be found here. For more information or to interview a trial investigator, contact Claire Crye at 281.825.9927 or Claire.Crye@usoncology.com or Edie DeVine at 209.814.9564 or Edie.DeVine@gcihealth.com.
###
About US Oncology Research
US Oncology Research draws from a network of experienced investigators and dedicated clinical staff who specialize in oncology clinical trials. US Oncology Research serves approximately 60 research sites and more than 165 locations, managing about 400 active trials at any given time. For the past 20 years, physicians in the research network have enrolled more than 82,000 patients in over 1,600 trials and have played a role in more than 100 FDA-approved cancer therapies. US Oncology Research is supported by McKesson Corporation.
About The US Oncology Network
Every day, The US Oncology Network (The Network) helps more than 1,380 independent physicians deliver value-based, integrated care to patients — close to home. Through The Network, these independent doctors come together to form a community of shared expertise and resources dedicated to advancing local cancer care and to delivering better patient outcomes. The Network provides practices with access to coordinated resources, best business practices, and the experience, infrastructure and support of McKesson Corporation. This collaboration allows the providers in The Network to focus on the health of their patients, while McKesson focuses on the health of their practices. The Network is committed to the success of independent practices, everywhere.
Contacts
US Oncology Research
Claire Crye, Public Relations
281.825.9927 claire.crye@usoncology.com
GCI Health on behalf of US Oncology Research
Edie DeVine, Public Relations
209.814.9564 edie.devine@gcihealth.com
Community-based practices in The Network advance value-based care by significantly reducing costs while enhancing care
THE WOODLANDS, TEXAS, Nov. 11, 2020—The US Oncology Network (The Network) reached a major milestone recently in its journey to provide high-quality, value-based care to local communities by enrolling its 100,000th patient in the Centers for Medicare & Medicaid Innovation’s (CMMI) Oncology Care Model (OCM). In realizing this goal, the participating Network practices delivered more than $122 million in cumulative savings to Medicare over the program’s first six performance periods (PP). The OCM is a five-year pilot program developed by CMMI to provide higher quality, more coordinated cancer care at the same or lower cost to Medicare. The program is part of Medicare’s ongoing effort to move healthcare to a system based on value rather than volume.
“We are very excited to enroll our 100,000th patient in the Oncology Care Model while also providing over $100 million in cumulative savings to Medicare,” said Michael Seiden, MD, PhD, president, The US Oncology Network. “These achievements showcase the ability of practices in The Network to consistently perform well in the OCM while demonstrating that high-quality care and cost management can work in tandem to provide value to all stakeholders.”
The OCM is a very large, complex program that requires enhanced patient care, effective cost management and comprehensive clinical data reporting to Medicare, to highlight only a few key elements of the program. Practices across The Network are performing well in the OCM, and most have shown improvement for each subsequent performance period.
“Celebrating our 100,000th OCM patient and seeing better performance each period remind us that success is an ongoing process,” said Beatrice Mautner, vice president of Clinical & Innovent Services, The US Oncology Network. “We are continually striving to be at the forefront of value-based care by constantly developing innovative resources and solutions to challenges as they arise, empowering community oncology to lead the way forward and succeed in this new environment.”
At the end of the most recent OCM performance period, PP6, significant gains occurred in critical performance areas across the participating Network practices, resulting in:
Improved quality compared to baseline performance during Performance Period 1
- Hospitalizations reduced by 7 percent
- Emergency department visits decreased by 3 percent
- Hospice utilization increased by 5 percent
Increased focus on pain and depression management
- The pain level of 94 percent of patients was captured and a plan implemented for elevated pain control
- 80 percent of patients who reported depression were screened and given strategies for improvement
Enhanced patient experience and services
- Shared decision making with patients became a priority at the start of treatment
- Patients received a comprehensive treatment plan explained by the physician
- Access to care was improved with “Call Us First” campaigns, proactive high-risk outreach, enhanced triage, electronic patient-reported outcomes and same day/next morning urgent care access
- Increased support and care coordination were provided through highly trained navigators and social workers
“The impressive results achieved by The Network is a testament to the commitment by the practices to deliver high-quality, value-based care,” said Marcus Neubauer, MD, chief medical officer, The US Oncology Network. “Enrolling 100,000 patients into the OCM and earning high performance marks during PP6 are proof that the participating Network practices are major contributors to this program by providing quality care and saving healthcare dollars.”
Although many practices participating in the OCM are still looking for a path to success, those in The Network have succeeded in part because they have access to comprehensive, proven resources that have helped them successfully transition to value-based care. These resources include industry-leading technologies that drive evidence-based decision-making at the point of care, advanced analytics for optimal data management and reporting, and innovative pharmacy solutions for efficient drug management. The Network, supported by McKesson, also provides practices access to thought leaders and key staff who have deep expertise in the OCM and value-based care.
“At least 50 percent of The Network practices participating in the OCM have chosen two-sided risk for 2020,” noted Stuart Staggs, senior director of Strategic Programs, McKesson. “This demonstrates a very high level of confidence in the support they are receiving from The Network and McKesson that enables them to successfully meet the complex challenges the OCM presents.”
The US Oncology Network is committed to ensuring community practices have access to all the resources necessary to successfully accomplish the massive practice transformation required by value-based and alternative payment models. To learn more, visit usoncology.com.
###
About The US Oncology Network
Every day, The US Oncology Network (The Network) helps more than 1,380 independent physicians deliver value-based, integrated care to patients — close to home. Through The Network, these independent doctors come together to form a community of shared expertise and resources dedicated to advancing local cancer care and to delivering better patient outcomes. The Network provides practices with access to coordinated resources, best business practices, and the experience, infrastructure and support of McKesson Corporation. This collaboration allows the providers in The Network to focus on the health of their patients, while McKesson focuses on the health of their practices. The Network is committed to the success of independent practices, everywhere.
Contact
The US Oncology Network
Claire Crye, Public Relations
281.825.9927 claire.crye@usoncology.com
By uniting with The Network, Alliance Cancer Specialists and Northwest Oncology strengthen their ability to deliver advanced cancer care in local communities
THE WOODLANDS, Texas, Oct. 22, 2020— The US Oncology Network (The Network), the largest organization of its kind dedicated to advancing local cancer care and better patient outcomes, continues to expand its reach into local communities by welcoming Alliance Cancer Specialists and Northwest Oncology. The addition of these two independent and physician-owned practices strengthens the availability of advanced cancer care services in communities across Southeastern Pennsylvania and Northwest Indiana while extending the reach of The US Oncology Network.
“Adding these premier cancer practices to our organization is an exciting development, as it marks the continued growth and expansion of The Network into more local communities,” said Michael V. Seiden, MD, PhD, president, The US Oncology Network. “Both practices are regional leaders in advanced, integrated care who will bring new expertise and fresh ideas to The Network, enhancing our ability to serve patients close to home. We look forward to collaborating with these highly skilled specialists to advance cancer care in local communities, helping us achieve our mission of preserving and strengthening community oncology.”
As a leader at the forefront of community oncology, The US Oncology Network is committed to ensuring community-based oncology practices remain strong and viable in the evolving healthcare landscape. Today almost 42 percent of patients battling cancer receive treatment in a community setting.* Community oncology brings many benefits and value to healthcare, and as the COVID-19 pandemic sweeps across the nation, the availability of high-quality, affordable local care becomes even more critical. Rather than having to travel long distances for care, patients receiving treatment in community practices have convenient, easy access to comprehensive, multidisciplinary care that includes some of the most cutting-edge, promising therapies available today. Patients also gain other benefits. Many practices have their own pharmacies that dispense oral therapies and chemotherapy drugs, enabling greater continuity of care and better drug therapy management. Care in a community-based practice is also more cost-effective than most other settings. This is an important advantage for patients who are paying a greater percentage of out of pocket costs, as well as for payers.
The US Oncology Network empowers community practices to deliver these benefits in a variety of ways. As part of The Network, Alliance Cancer Specialists and Northwest Oncology gain access to the expertise, industry-leading technologies and vast resources of The Network to help them drive high-quality care and strengthen operational efficiencies in the value-based environment. They can collaborate with an expanded physician community of more than 1,350 physicians and clinicians who share expertise and best practices through committees, workshops and conferences. The practices also gain access to Value Pathways powered by NCCN™—evidence-based treatment guidelines developed by physicians and clinicians in The Network along with the National Comprehensive Cancer Network®.
Alliance Cancer Specialists serves patients in Southeastern Pennsylvania, with 21 board-certified medical oncologists and hematologists, eight advanced practice providers and approximately 160 employees who serve patients and referring physicians in the Delaware Valley from 10 sites of service. The practice leverages the combined strength and broad expertise of its oncologists to administer the full range of state-of-the-art cancer treatments. The care team also includes oncology certified nurses, laboratory technologists and support staff who are committed to providing the highest quality of personalized care and support to patients.
“Providing high-quality, advanced cancer care to patients in their local community has always been the focus of our practice,” said Allen Terzian, MD, practice president, Alliance Cancer Specialists. “By partnering with The Network, our independent practice can continue to thrive in this evolving healthcare landscape. We look forward to future collaborations with our colleagues in The US Oncology Network including our neighbors, Consultants in Medical Oncology and Hematology (CMOH). Uniting our community-based oncology services with The Network heightens our ability to offer patients cutting-edge, evidence-based treatments that provide the best opportunity for optimal outcomes.”
Northwest Oncology is an integrative healthcare center specializing in the diagnosis, treatment and support of patients with oncolytic and hematological disorders. The practice is an advanced oncology group in Northwest Indiana with eight physicians and a team of more than 40 support staff members who provide medical oncology, hematology and gynecologic oncology services from two locations. Utilizing an integrative team approach, the practice collaborates with geneticists, radiation oncologists, surgeons and primary care physicians to provide high-quality, comprehensive care close to home.
“Joining The US Oncology Network not only gives our patients access to novel therapies and supportive care programs that offer the best possible outcomes and quality of life, it also enables us to tap into a wide range of resources that can help us remain independent and viable in today’s challenging healthcare landscape,” noted Mohamad Kassar, MD, practice president, Northwest Oncology.
To learn more about how The US Oncology Network supports community-based oncology, visit www.usoncology.com.
*https://communityoncology.org/wp-content/uploads/2017/08/What-is-Comm-Onc.pdf
###
About The US Oncology Network
Every day, The US Oncology Network (The Network) helps more than 1,350 independent physicians deliver value-based, integrated care to patients — close to home. Through The Network, these independent doctors come together to form a community of shared expertise and resources dedicated to advancing local cancer care and to delivering better patient outcomes. The Network provides practices with access to coordinated resources, best business practices, and the experience, infrastructure and support of McKesson Corporation. This collaboration allows the providers in The Network to focus on the health of their patients, while McKesson focuses on the health of their practices. The Network is committed to the success of independent practices, everywhere.
Contact
The US Oncology Network
Claire Crye, Public Relations
281.825.9927 claire.crye@usoncology.com
Chief Scientific Officer of US Oncology Research honored for groundbreaking achievements in gynecologic oncology
THE WOODLANDS, Texas, Oct. 6, 2020 — Robert L. Coleman, MD, FACOG, FACS, chief scientific officer of US Oncology Research, has been named an inductee to the 2020 class of the OncLive® Giants of Cancer Care®. Now in its eighth year, Giants of Cancer Care is a recognition program celebrating individuals whose achievements have propelled global oncology forward and made remarkable differences in patient care and research. In a virtual ceremony on November 5, Dr. Coleman will receive the award for Gynecological Malignancies, recognizing his many achievements which have established the building blocks for future advancement in the field.
“The members of the 2020 class of Giants of Cancer Care are oncology legends who have made remarkable differences in the cancer care landscape,” said Mike Hennessy, Jr., president and CEO of MJH Life Sciences™, the parent company of OncLive — a multimedia platform connecting healthcare professionals to the latest in oncology advancements, news and resources. Out of 818 nominations, only 15 oncologists were selected as inductees to the 2020 Giants of Cancer Care for their achievements in specialties spanning the field, from breast cancer and melanoma to cancer diagnostics and translational science.
An internationally recognized leader in ovarian, uterine and cervical cancer research, Dr. Coleman has played a key role in developing some of the most promising treatments available today for gynecological cancer management. “I couldn’t be prouder to see Dr. Coleman take his place among the Giants of Cancer Care, a recognition that honors his extraordinary contributions to clinical research in gynecological malignancies,” said Michael Seiden, MD, PhD, president of The US Oncology Network. “His work exploring the role of novel therapies such as PARP inhibitors for ovarian cancer, as well as surgical approaches to ovarian cancer management, continues to make an impact in the lives of patients.”
Dr. Coleman joined The US Oncology Network (The Network) in March 2020, named as chief scientific officer and leader of US Oncology Research, The Network’s clinical research arm. The US Oncology Network, which is supported by McKesson Corporation, is one of the nation’s largest networks of integrated, community-based oncology practices dedicated to advancing high-quality, evidence-based cancer care. “Being inducted into the OncLive Giants of Cancer Care is a great honor, and I’m humbled and inspired to join this group of luminaries in the field of oncology research and care,” Dr. Coleman said. “No cancer researcher works alone, and I’d like to acknowledge and thank the many collaborators working with me to move oncology forward and improve patients’ lives. These are dynamic times for cancer research, and I couldn’t be more excited to continue this critical work with my US Oncology Research colleagues.”
The 8th Annual Giants of Cancer Care virtual awards ceremony will take place on Thursday, November 5, 2020, at 7:30 p.m. EST. It’s free to register for the virtual ceremony, which will be available on demand at giantsofcancercare.com after the conclusion of the event. To learn more about the event and the 2020 class of Giants of Cancer Care, read the OncLive press release.
###
About US Oncology Research
US Oncology Research draws from a network of experienced investigators and dedicated clinical staff who specialize in oncology clinical trials. US Oncology Research serves approximately 60 research sites and more than 165 locations, managing about 400 active trials at any given time. For the past 20 years, physicians in the research network have enrolled more than 80,000 patients in over 1,600 trials and have played a role in more than 100 FDA-approved cancer therapies. US Oncology Research is supported by McKesson Corporation.
Media Contacts
US Oncology Research
Claire Crye
281.825.9927
Claire.Crye@usoncology.com
Inclusion of the CRESTONE Study within the Selected Trials for Accelerated Rollout Program will enhance patient recruitment and facilitate local site participation for patients with tumors harboring an NRG1 Gene Fusion
NEW YORK, NY and THE WOODLANDS, Texas, Sept. 30, 2020—Elevation Oncology, a clinical stage biopharmaceutical company focused on the development of precision medicines for patients with genomically defined cancers, and US Oncology Research, one of the largest community-based oncology site management organizations in the U.S., announced today a collaboration to utilize the US Oncology Research Selected Trials for Accelerated Rollout (STAR) program for patient enrollment in the registration-enabling Phase 2 CRESTONE study for patients with solid tumors of any origin that have an NRG1 gene fusion.
“The ability to accurately detect rare genomic driver alterations in a patient’s tumor and subsequently open up a clinical study site in response, is paramount to bringing precision therapy opportunities to patients that may benefit from treatment,” said Shawn Leland, PharmD, RPh, founder and chief business officer of Elevation Oncology. “US Oncology Research is ideally positioned to expand the reach of the CRESTONE study for patients with cancers harboring an NRG1 gene fusion for investigational treatment with seribantumab. A key component of this collaboration is the ability to quickly open CRESTONE clinical trial sites via the US Oncology Research STAR program, which minimizes patient travel and disruption in clinical care, a major advantage particularly given the current travel complexities due to COVID-19.”
The STAR program opens and activates clinical trials quickly across all cancer research sites managed by US Oncology Research. STAR is an operational model that allows for pre-screening of potentially eligible subjects upfront and only opens sites where subjects are identified. When a potential STAR trial patient is identified at a facility, the practice is trained in the details of the trial, and the study is opened within a two-week timeframe at the location where the patient will be treated.
“Advancements in diagnostic testing, and an evolution in the understanding of cancer development and progression, have enabled the identification of driver mutations and subsequent treatment for patients with cancer that no longer is associated with the tissue of origin for a particular disease,” said Robert L. Coleman, MD, chief scientific officer of US Oncology Research. “Given the broad reach of US Oncology Research, we are able to provide access to investigational treatments at a local medical center and rapidly open up clinical study sites in order to provide options for our patients and physicians in their clinical treatment decisions across the country. With close collaboration between our individual cancer specialists, we are creating a future where cancers that are defined by genomic driver alterations can be rapidly identified and matched to treatments that may be able to stop the growth of an individual patient’s disease, wherever they may live.”
US Oncology Research enables practices to offer patients access to the latest cancer clinical trial options in their local communities, providing the opportunity for better outcomes while contributing to the advancement of cancer treatment. US Oncology Research serves approximately 60 research sites and more than 165 locations, managing about 400 active trials at any given time. This breadth of coverage, and commitment to cross-disciplinary collaboration among facilities and individual specialties, makes US Oncology Research uniquely situated to accelerate the clinical development of precision medicines that target rare genomic alterations.
Patients and physicians can learn more about the CRESTONE study at www.nrg1fusion.com or on www.ClinicalTrials.gov under the NCT number NCT04383210.
###
About Elevation Oncology
Elevation Oncology is founded on the belief that every patient with cancer deserves to know what is driving the growth of their disease and have access to therapeutics that can stop it. We make genomic tests actionable by selectively developing drugs to inhibit the specific alterations that have been identified as drivers of disease. Together with our peers we work towards a future in which each unique test result can be matched with a purpose-built precision medicine to enable an individualized treatment plan for each patient. Our lead candidate, seribantumab, inhibits tumor growth driven by NRG1 fusions and is currently being clinically tested in the Phase 2 CRESTONE study for patients with tumors of any origin that have an NRG1 fusion. Details on CRESTONE are available at www.NRG1fusion.com. For more information visit www.ElevationOncology.com.
About US Oncology Research
US Oncology Research draws from a network of experienced investigators and dedicated clinical staff who specialize in oncology clinical trials. US Oncology Research serves approximately 60 research sites and more than 165 locations, managing about 400 active trials at any given time. For the past 20 years, physicians in the research network have enrolled more than 80,000 patients in over 1,600 trials and have played a role in more than 100 FDA-approved cancer therapies. US Oncology Research is supported by McKesson Corporation.
About Seribantumab and NRG1 Gene Fusions
Seribantumab is a fully human IgG2 monoclonal antibody that binds to human epidermal growth factor receptor 3 (HER3). HER3 is traditionally activated through binding of its primary ligand, neuregulin-1 (NRG1). The NRG1 gene fusion is a rare genomic alteration that combines NRG1 with another partner protein to create chimeric NRG1 “fusion proteins”. The NRG1 fusion protein is often also able to activate the HER3 pathway, leading to unregulated cell growth and proliferation. Importantly, NRG1 gene fusions are mutually exclusive with other known driver mutations and are considered a unique oncogenic driver event essential for tumor cell survival.
NRG1 fusions have been identified in a variety of solid tumors, including lung, pancreatic, gallbladder, breast, ovarian, colorectal, neuroendocrine, and sarcomas. In preclinical experiments, seribantumab prevents the activation of HER3 signaling in cells that harbor an NRG1 gene fusion. In addition to extensive nonclinical characterization and testing, seribantumab has been administered to 847 patients across 12 phase 1 and 2 studies, both as a monotherapy and in combination with various anticancer therapies. Seribantumab is currently being clinically tested in the Phase 2 CRESTONE study for patients with solid tumors of any origin that have an NRG1 fusion.
About the CRESTONE Study
Clinical Study of Response to Seribantumab in Tumors with Neuregulin-1 (NRG1) Fusions. CRESTONE is a Phase 2 tumor-agnostic “basket trial” of seribantumab in patients with any solid tumor that harbors an NRG1 fusion. The primary objective of the study is to describe the anti-tumor activity and safety of seribantumab specifically in patients with an NRG1 gene fusion. CRESTONE offers a clinical trial opportunity for patients with advanced solid tumors who have not responded or are no longer responding to treatment. Patients are encouraged to talk to their doctor about genomic testing of their tumor. CRESTONE is open and enrolling today in the US. For more information visit www.NRG1fusion.com.
Media Contacts
Elevation Oncology
David Rosen, Argot Partners
716.371.1125
media@ElevationOncology.com
US Oncology Research
Claire Crye
281.825.9927
Claire.Crye@usoncology.com
Available in patients’ own communities, novel clinical trials are making an impact in the fight against cancer
THE WOODLANDS, Texas, Sept. 29, 2020 — US Oncology Research, one of the largest community-based oncology research programs in the U.S. one of the largest community-based oncology research programs in the U.S. one of the largest community-based oncology research site management organizations in the U.S., is celebrating the significant milestone of contributing to the FDA approval of over 100 cancer therapies. This achievement is a result of the hard work and dedication to research from more than 165 research locations conducting over 1,600 clinical trials for cancer therapy. More than 80,000 participants have enrolled in clinical trials since 1999.
“US Oncology Research’s core mission is to bring potentially life-saving and life-improving treatments to the community where patients seek care,” said Robert L. Coleman, MD, FACOG, FACS, chief scientific officer, US Oncology Research. “These new interventions come from expert stewardship and execution of clinical research protocols positioned to better understand cancer biology and challenge the status quo. We are, therefore, incredibly proud of this milestone, which reflects the dedication and collective spirit of investigators across The US Oncology Network, committed to defining the next treatment standard. Research is a team sport dedicated to the individual patient.”
With each approved therapy, real patient stories reflect the hope and potential that new science brings. One such patient is Henry “Ray” Picagli, who consulted with his oncologist, James H. Essell, MD, at Cincinnati-based OHC (Oncology Hematology Care), after his lymphoma returned after chemotherapy. “Dr. Essell told us about the CAR-T clinical trial OHC was offering for patients in my exact situation and that he thought I would be a good candidate for the investigational treatment,” said Picagli. “I was immediately all-in for two reasons. Obviously, I want to live, but I also want others to benefit from what I’m doing, even if it helps only one person.”
Today, Ray’s scans are clear, and he is in remission. “I spoke with friends in the medical field,” added Picagli. “Everyone said the same thing: ‘You have no idea how lucky you are to be able to get this investigational treatment and that it’s available at OHC. And they were right.’”[i]
OHC is one of 68 community-based practices in The US Oncology Network, including about 482 sites of care and more than 1,350 physicians, many of which offer their patients a chance to participate in advanced clinical trials. “Usually available only in major academic medical centers or hospital systems, these novel cancer trials are accessible to patients close to home, right in their own communities,” said Michael Seiden, MD, PhD, president of The US Oncology Network. “With about 400 active trials at any given time, US Oncology Research is making a tangible difference in the lives of patients.”
Having access to a state-of-the-art clinical trial has made all the difference for Laura Reith, who was diagnosed with stage IV triple negative breast cancer just months after delivering a baby. “I wanted to stay closer to home so I could continue with my life,” said Reith, who enrolled in a trial under the guidance of her physicians at Illinois Cancer Specialists (ICS), a practice in The US Oncology Network. “I work full-time. I have small kids. It would be difficult to spend a full day in a hospital hours away.” Now in her 39th round of treatment in the trial, which she started in 2018, she shows no signs of disease.[ii]
“It’s all about having the right advocate in your corner. I’m so thankful to have a team of physicians that cares about more than just the dollars – they care about not only my journey but about the future,” said Reith. “Being on a clinical trial has provided me hope above all. Hope for more time with my kids. Hope for a future without cancer.”
###
About US Oncology Research
US Oncology Research draws from a network of experienced investigators and dedicated clinical staff who specialize in oncology clinical trials. US Oncology Research serves approximately 60 research sites and more than 165 locations, managing about 400 active trials at any given time. For the past 20 years, physicians in the research network have enrolled more than 80,000 patients in over 1,600 trials and have played a role in more than 100 FDA-approved cancer therapies. US Oncology Research is supported by McKesson Corporation.
[i] This patient’s experience may be atypical and individual results may vary. The Surveillance, Epidemiology, and End Results (SEER) database, which tracks 5-year relative survival rates in the United States, lists survival rates of 73% for localized, 72% for regional, 55% for distant and 63% for all SEER stages of non-Hodgkin lymphoma combined. https://www.cancer.org/cancer/non-hodgkin-lymphoma/detection-diagnosis-staging/factors-prognosis.html
[ii] This patient’s experience may not be typical and individual results may vary. The SEER database lists survival rates of 99% for localized, 86% for regional, 27% for distant and 90% for all SEER stages of breast cancer combined. https://www.cancer.org/cancer/breast-cancer/understanding-a-breast-cancer-diagnosis/breast-cancer-survival-rates.html
A recognized leader in radiation oncology, Dr. Kavadi brings extensive experience in patient care, research and operations to The Network
THE WOODLANDS, Texas, Aug. 4, 2020 — Vivek S. Kavadi, MD, FASTRO, a nationally known expert in the field of radiation oncology, has been named chief radiation oncology officer for The US Oncology Network (The Network). Dr. Kavadi will lead the development of clinical strategies and best practices to advance the delivery of cutting-edge radiation therapies across The Network, as well as spearhead new initiatives in radiation oncology that empower practices to thrive in the challenging value-based care environment.
“Dr. Kavadi is a nationally recognized expert in radiation oncology and a well-respected physician-leader within The Network,” said Michael Seiden, MD, PhD, president, The US Oncology Network. “He has extensive experience that spans patient care, research and operations and has an in-depth knowledge of The Network, having served as chairman of the radiation executive committee and medical director of radiation oncology. We are very excited Dr. Kavadi will now lead our efforts to advance radiation therapy and integrated care while continuing to drive the critical role The Network is playing in the transition to value-based care.”
Dr. Kavadi has been a practicing radiation oncologist for nearly 30 years, most recently treating patients at Texas Oncology. As a member of the Board of Directors of Texas Oncology―a practice in The Network with more than 200 sites of service―Dr. Kavadi has in-depth experience in building and managing high performing radiation oncology departments. Board certified in radiation oncology, he has a clinical interest in prostate and breast cancer and is Primary Investigator for The US Oncology Network RTOG Affiliation. Dr. Kavadi graduated from Rice University and received his medical degree from Harvard Medical School. He then completed a transitional internship at Baylor College of Medicine and a residency in radiation oncology at M.D. Anderson Cancer Center where he was chief resident. He is currently pursuing an MBA at the Wharton School.
“Dr. Kavadi is a highly regarded leader in radiation oncology, and we are honored he has chosen to join our team,” said Marcus Neubauer, MD, chief medical officer, The US Oncology Network. “He brings extraordinary leadership skills and clinical expertise in radiation oncology to our organization. I look forward to collaborating with him on initiatives to empower The Network practices to thrive in today’s evolving landscape.”
Dr. Kavadi has received many accolades throughout his career and was recently named a fellow by the American Society for Radiation Oncology (ASTRO), a recognition usually only awarded to radiation oncologists working in academic settings rather than private practice. He was recognized by ASTRO for his leadership, service, research, patient care and educational contributions to the organization, as well as the field of radiation oncology.
“Joining The Network in this capacity provides a wonderful opportunity to meet the goals I have always had throughout my career―to deliver high-quality cutting-edge care, to contribute to the advancement of my field and to provide meaningful leadership when the opportunity arose,” said Dr. Kavadi. “The US Oncology Network is a world-class organization with tremendous resources that is dedicated to enhancing cancer care across local communities, and I look forward to contributing to this worthwhile goal.”